New malaria vaccines that helped Ghana significantly reduce child deaths were stalled after Trump and others cut aid.

New vaccines are bringing Ghana closer to its long-standing goal of ending child deaths from malaria, showing the promise of these shots in fighting a disease that takes the lives of nearly half a million young children in Africa each year, according to the international vaccine aid group Gavi and the country’s health service.
Gavi told Reuters that cuts in aid from the Trump administration and other wealthy governments could result in fewer children receiving help in the continent most affected by malaria.
Ghana is among the countries that had already made significant progress reducing malaria mortality by scaling up interventions such as the distribution of bed nets treated with insecticides and improving access to both preventive drugs and prompt treatment.
According to Dr. Selorm Kutsoati, who leads Ghana’s immunisation programme, two new vaccines—one from British drugmaker GSK (GSK.L) and another from Oxford University in collaboration with the Serum Institute of India—are helping to close the remaining gap.

Vials of the RTS,S malaria vaccine, also known as Mosquirix, are stored inside a fridge at the Mother and Child Hospital in Kasoa, Ghana. REUTERS/Francis Kokoroko
“For me, the malaria vaccine is a gamechanger,” she told Reuters.
Gavi is currently the sole organization buying malaria vaccines for African countries. It expects to spend just over $800 million on the program over the next five years—about 28% less than what’s needed—after falling $2.9 billion short of its overall funding target for the period, according to internal estimates prepared for its board in December and reviewed by Reuters.
The U.S. “remains committed to working with global partners to combat malaria,” a Department of Health and Human Services official told Reuters.
According to an official, the Trump administration won’t release funds to Gavi unless it begins phasing out vaccines that use the mercury-based preservative thimerosal. Anti-vaccine groups have connected thimerosal to autism and other neurodevelopmental disorders, even though numerous studies have found no evidence of related safety concerns.
Gavi confirmed the request and said the group remained in contact with the U.S. government on the subject. Any decision related to its portfolio would be “guided by scientific consensus,” it said.
Other donors have also been scaling back support. Britain, Gavi’s biggest donor, has pledged 1.25 billion pounds ($1.72 billion) over the next five years, more than 20% less than for 2020-25.
Britain’s international development minister, Jenny Chapman, said the country remains committed to supporting Gavi’s work because it saves lives.
Some major global organisations initially doubted the potential of the two vaccines now being rolled out in 24 African countries with help from Gavi.
According to clinical trials, the World Health Organization (WHO) estimates that three shots can cut malaria cases by more than 50% in the first year, though this is less effective than many common childhood vaccines. To keep protection going, a fourth dose is needed before a child turns two.
Supporters of the vaccines point to the success in Ghana, saying even a partially effective shot has translated into many lives saved.
“In real-world settings, we’re seeing significant impact,” Gavi’s Gordon said.
In Ghana, confirmed deaths among children under 5 have fallen by nearly 86%, dropping from 245 in 2018—the year before GSK’s vaccine was introduced in select districts—to just 35 in 2024, according to government data. Kutsoati noted that a decade ago, nearly 1,000 children in that age group died each year..
Malaria infections have also declined, from roughly 6.7 million in 2018 to 5.3 million in 2024, around a fifth of which were among children under 5, Ghana’s figures show.
The actual numbers are likely to be higher, as many malaria cases do not get diagnosed, and deaths that occur at home often go unreported, said Dorothy Achu, the WHO’s team lead for malaria in Africa. There can also be inconsistent reporting by some health facilities.
But Achu agreed the combination of strategies used in Ghana resulted in a “significant reduction in malaria deaths”, adding the WHO is using the country’s figures to update its estimates.
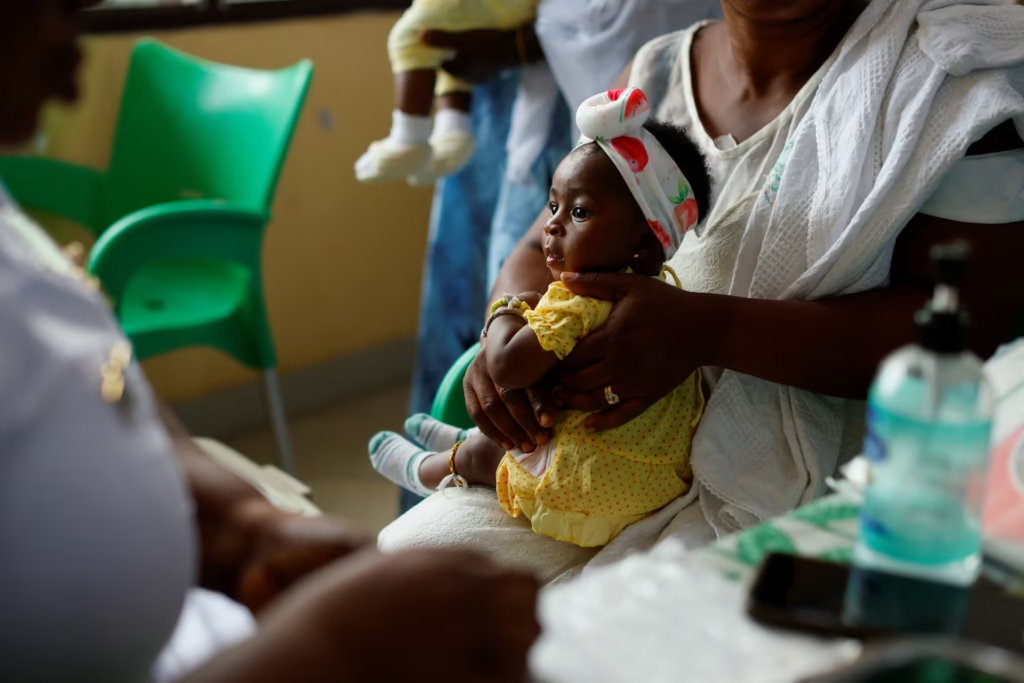
Esther Kolan, a 31-year-old clothing trader, did not need much persuading to get her 1-year-old son Phenehas Gyngyi Jr. vaccinated last summer at the Mother and Child Hospital in the southern town of Kasoa.
Her brother died of malaria just before his 15th birthday. A daughter was hospitalised twice with the disease before she turned 3.
“I told myself, no matter the condition, I have to go for the vaccine,” Kolan said, adding her family also sleeps under bed nets.
Phenehas has had three doses and has never been hospitalised with malaria.
“This has really helped me a lot,” said Kolan, who plans to get him a booster shot soon. “I was not scared for my child.”
Malaria deaths were already declining in their district when vaccines became available in 2023, according to Stanley Yaidoo, the municipal health services director. But the number of cases still put pressure on hospitals, exhausting staff and taking up beds that could be used to treat other dangerous diseases, he told Reuters.
“The vaccine implementation was the master stroke that we needed to support the already existing interventions,” Yaidoo said.

Some regions managed to eliminate malaria without a vaccine, but countries in sub-Saharan Africa face particular challenges, disease experts say.
Many are among the world’s poorest, with poorly-resourced health systems. The prevailing strain is particularly deadly, and there is growing resistance to preventive and curative drugs. Control efforts have been disrupted by conflicts and natural disasters.
The first countries to use the vaccines – Kenya, Malawi and Ghana – were part of a WHO-led pilot programme that began in 2019 with GSK’s shot. The WHO approved this vaccine for wider use in 2021, but the rollout faced hurdles, including a vast supply shortfall.
Access improved when WHO recommended the Oxford shot in 2023.
In many countries, it is too early to assess the vaccines’ impact. But there are anecdotal reports of reductions in cases, hospitalisations and deaths among young children, according to the Gavi documents and interviews with health officials in four countries.
Take-up of the vaccines has varied, the documents show. In the first six months of 2025, coverage rates across 11 countries for three doses ranged from over 70% in Ghana and Burkina Faso, to 45% in Liberia and 35% in conflict-hit South Sudan.
Introducing a new vaccine that requires multiple doses has presented logistical challenges, especially in rural areas where transportation and storage options are limited.
In Ghana, there was also resistance from a number of traditional and religious leaders, and politicians skeptical about the benefits, Yaidoo told Reuters.
But results talk, he said.
“Those who have had the vaccination, they give their testimonies on how their children are protected from severe malaria. So many of them are actually our ambassadors.”
Cases of severe malaria among vaccinated children were 58% lower than among unvaccinated children in the year after they received the third dose across the countries that participated in the pilot, a study published in The Lancet medical journal in January found.
Health officials in Kenya and Malawi did not respond to Reuters’ questions about their vaccination programmes.
At least four more countries plan to introduce malaria vaccines before 2028, Gavi said.
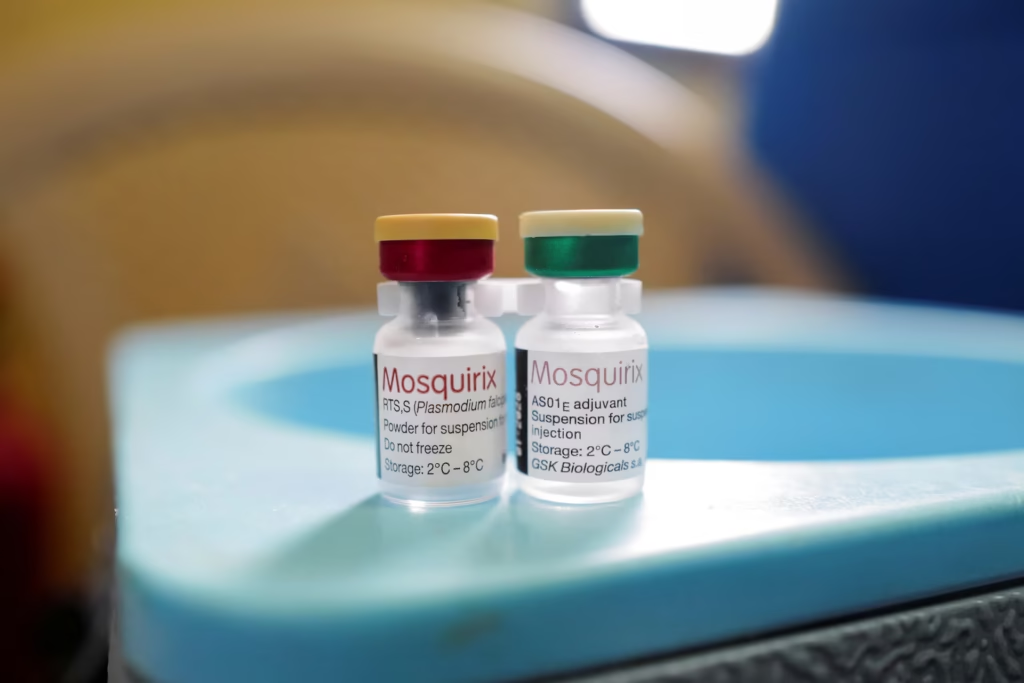
Vials of the RTS,S malaria vaccine, also known as Mosquirix, at the Mother and Child Hospital in Kasoa, Ghana. REUTERS/Francis Kokoroko/Illustration
Until this year, Gavi could subsidise 85% of the assessed need for shots in areas of medium and high malaria transmission, with governments contributing as little as $0.20 per dose.
It has now reduced its spending cap to 70% for areas that will be ordering shots for the first time, the documents show. It will also be asking all but the poorest governments to increase their contributions, which vary depending on the strength of their economies.
Details of how these changes will affect individual countries are being worked out, Gavi said.
Lowering vaccine prices could help offset the impact of reduced aid. In June, GSK and its partner, India’s Bharat Biotech, announced plans to cut the price of their shot to under $5 per dose by 2028, about half the current cost. Then in November, Gavi and UNICEF struck a deal to pay 25% less for Serum’s vaccine, which is now priced at around $4 per dose, within about a year.
GSK said the real-world data was encouraging, and it was working with Gavi on how to make the roll-out as effective as possible. It did not elaborate. The other companies did not respond to requests for comment.
At least three countries – Burkina Faso, Ivory Coast and Togo – have committed to covering some malaria vaccine needs themselves, Gordon said.
But Tanzania is struggling to plug funding gaps and will have to delay the start of its vaccination campaign, said Dr Samwel Lazaro, acting head of its malaria programme.
“Currently, the government is focused on ensuring the implementation of the most essential and life-saving services, such as the use of medicated bed nets,” Lazaro said.
($1 = 0.7255 pounds)
